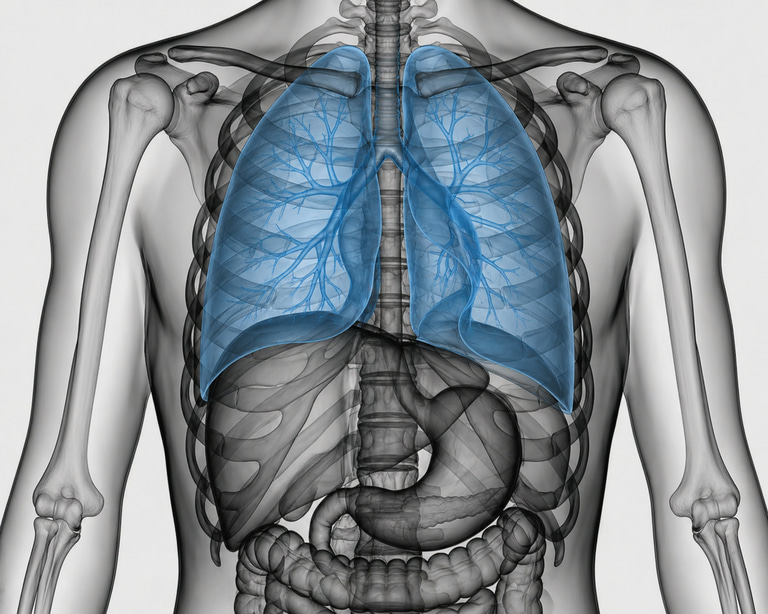
CT of the lungs, also referred to as CT chest or computed tomography of the lungs, is a high-resolution radiological examination that enables detailed visualization of the lung parenchyma, airways, pleura, and intrathoracic structures. “CT” and “computed tomography” refer to the same imaging modality. By combining X-ray radiation with advanced computer processing, cross-sectional images with a high degree of anatomical detail are generated, allowing detection of subtle abnormalities within the lungs and thorax.
This modality has significantly higher diagnostic accuracy compared with conventional chest radiography and is widely used to identify both early and advanced pathological changes. CT of the lungs plays a central role in the evaluation of respiratory symptoms and may facilitate early detection of serious conditions where timely diagnosis is critical for prognosis and management.
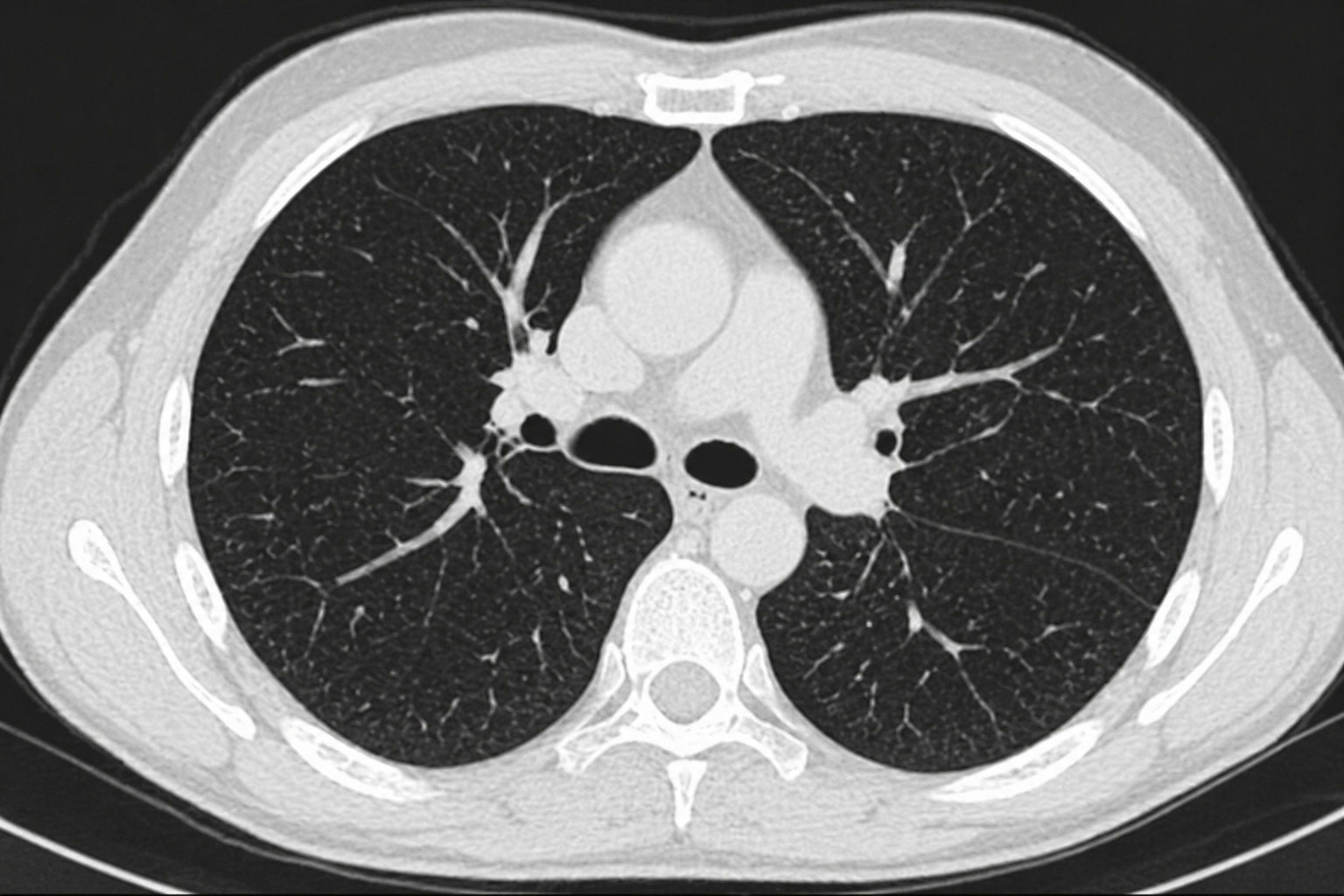
What can a CT scan of the lungs demonstrate?
CT imaging of the lungs is primarily used to assess structural, inflammatory, and neoplastic processes affecting the lungs and other thoracic structures. The diagnostic yield depends on the clinical indication, as well as the patient’s history and presenting symptoms.
Depending on the indication, CT may demonstrate:
- Solid or subsolid pulmonary nodules and lesions suspicious for malignancy.
- Metastatic disease in the setting of known or suspected primary cancer.
- Emphysematous changes and structural remodeling associated with chronic obstructive pulmonary disease (COPD).
- Interstitial lung diseases, including fibrotic and inflammatory patterns.
- Infectious and inflammatory conditions such as pneumonia or bronchiolitis.
- Pleural abnormalities, including pleural effusion and pleuritis.
- Mediastinal and hilar lymphadenopathy.
- Pneumothorax (air within the pleural space) and other acute thoracic conditions.
- Vascular pathologies such as pulmonary embolism on contrast-enhanced CT.
All findings are interpreted within a clinical context, taking into account symptoms, risk factors, and prior medical history. Many imaging findings may be benign or of limited clinical significance, while others may require further investigation or longitudinal follow-up. Minor abnormalities are relatively common and do not necessarily indicate serious disease.
When is a CT scan of the lungs indicated?
CT of the lungs is used in the evaluation of both acute and chronic respiratory or thoracic symptoms, particularly when prior investigations have been inconclusive.
- Persistent or unexplained cough.
- Dyspnea or reduced exercise tolerance without a clear cause.
- Chest pain or thoracic discomfort.
- Hemoptysis (coughing up blood).
- Recurrent or prolonged respiratory infections.
- Suspected lung cancer or metastatic disease.
- Evaluation of chronic lung conditions such as COPD or pulmonary fibrosis.
- Abnormal findings on chest X-ray.
- Risk factors such as current or prior smoking or known lung disease.
The examination may also be used for follow-up of previously identified abnormalities or to assess response to treatment.
Can CT of the lungs detect lung cancer?
CT imaging is one of the most sensitive modalities for detecting abnormalities within the lung parenchyma and is commonly used in the evaluation of suspected lung cancer. It can identify small pulmonary nodules that may not be visible on standard chest radiography.
However, it is important to note that not all pulmonary nodules are malignant. Small nodules are relatively common and are often benign. Assessment is based on factors such as size, morphology, interval growth, and the patient’s overall risk profile. When appropriate, follow-up imaging or further diagnostic work-up is recommended.
How is a CT scan of the lungs performed?
The examination is quick and non-invasive and typically takes approximately 10–15 minutes. The patient lies on a table that moves through the CT scanner while images are acquired in multiple planes. The actual image acquisition takes only a few seconds.
In certain cases, intravenous contrast material is administered to enhance visualization of vascular structures and to better differentiate between tissue types. This is particularly relevant when evaluating suspected malignancy or pulmonary embolism. The need for contrast is determined on an individual basis by the physician.
CT imaging involves exposure to ionizing radiation; however, protocols are optimized to use the lowest possible dose while maintaining diagnostic image quality.
Medical assessment is required prior to referral
A medical consultation by telephone with the referring physician is always conducted prior to the examination. During this consultation, your symptoms, medical history, and risk factors are carefully reviewed to ensure an appropriate and clearly defined clinical indication.
Only after this assessment is it determined whether CT of the lungs is indicated. If appropriate, a referral is then issued to a radiology department. This process ensures that the examination is medically justified and tailored to the relevant diagnostic question.
The scan is performed by radiology staff, and the images are interpreted by a board-certified radiologist. You will receive a formal medical report including the findings and, if applicable, recommendations for further investigation or follow-up.
Physician consultation is always included
The pre-examination consultation is an integral part of the diagnostic process. By correlating symptoms with clinical risk factors, the physician can determine whether CT is the most appropriate modality or if alternative investigations should be considered. This approach minimizes unnecessary imaging and enhances diagnostic precision and patient safety.
When is CT of the lungs not appropriate?
CT of the lungs is not always the first-line investigation and should not replace urgent medical evaluation in the presence of severe or acute symptoms. In cases such as sudden onset dyspnea, severe chest pain, or suspicion of a life-threatening condition, immediate medical attention is required.
CT is also not routinely used without a clearly defined clinical indication, unless specific risk factors justify further evaluation.
Note! The examination is currently available in Stockholm, Gothenburg, and Malmö.