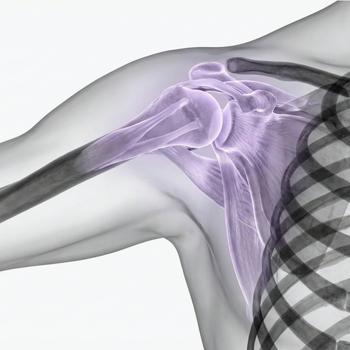
What is frozen shoulder?
Frozen shoulder, or adhesive capsulitis (also called “frozen shoulder”), is a condition in which the shoulder joint capsule becomes inflamed, thickened and stiff. This leads to a gradual decrease in mobility in the shoulder joint, often in combination with pain. The condition usually develops gradually and can last for a long time, often between 1–3 years. The shoulder joint (glenohumeral joint) is surrounded by a thin capsule that is normally elastic and allows for a great deal of mobility. In frozen shoulder, an inflammatory process occurs that causes the capsule to shrink and become less flexible. This limits the space in the joint and affects both active and passive mobility.
What happens in the shoulder with frozen shoulder?
The underlying mechanism is a combination of inflammation and fibrotic changes in the shoulder joint capsule. In an early stage, inflammation occurs that causes pain, especially during movement and load. Over time, this leads to thickening and scarring (fibrosis), which makes the capsule stiff and less stretchable. At the same time, the volume of the joint decreases, which further limits the ability to move and leads to a characteristic stiffness in several directions of movement.
Symptoms of frozen shoulder
The symptoms of frozen shoulder are characterized by a combination of pain and gradually increasing stiffness in the shoulder. Unlike many other shoulder disorders, where pain often dominates, it is precisely the pronounced limitation of mobility – both active and passive – that is typical of this condition. In the early stages, the symptoms can be difficult to distinguish from other shoulder problems, such as impingement or rotator cuff disorders. Over time, however, the stiffness becomes more prominent and affects everyday movements such as lifting the arm, getting dressed or reaching behind the back.
Frozen shoulder often develops in three phases, with symptoms changing over time:
Pain phase (“freezing”): Increasing pain in the shoulder, often worst at night and with movement. Mobility gradually begins to decrease.
Stiffness phase (“frozen”): Pain may decrease slightly, but stiffness is evident. Both active and passive mobility are severely limited.
Thawing phase: Mobility gradually improves and pain subsides.
Typical symptoms include the following:
Pain in the shoulder: Often diffuse and deep, may radiate down the upper arm.
Pronounced stiffness: Difficulty lifting the arm, rotating it or reaching behind the back.
Impaired function: Impact on everyday activities such as getting dressed or lifting objects.
Why do people get frozen shoulder?
The cause of frozen shoulder is not always completely understood, but the condition is often divided into a primary (idiopathic) and a secondary form. It is often a combination of biological changes in the tissue and external factors that affect the mobility of the shoulder over time.
Primary frozen shoulder occurs without a clear trigger and is most often seen in people between 40 and 60 years of age. It is thought to be linked to changes in the connective tissue, where the capsule becomes more prone to developing inflammation and fibrosis.
Secondary frozen shoulder, on the other hand, develops as a result of another event, such as a shoulder injury, surgery or a longer period of immobilization. Reduced movement in the joint can then trigger the inflammatory process that leads to stiffness.
There are also several known risk factors that increase the likelihood of developing the condition. Diabetes is strongly linked to frozen shoulder, likely through its effects on collagen and connective tissue. Thyroid diseases can also play a role by affecting tissue metabolism. Prolonged inactivity or limited use of the shoulder are additional factors that can contribute to the process starting and progressing.
How is frozen shoulder diagnosed?
The diagnosis is primarily based on a clinical examination where a clear limitation in both active and passive mobility is seen, especially in external rotation – which is one of the most typical findings in frozen shoulder. If necessary, imaging diagnostics can be used to exclude other causes of shoulder pain, such as rotator cuff rupture or other structural damage. A MRI of the shoulder can then provide a more detailed image of the joint capsule and other structures in the shoulder.
What can you do yourself? Treatment and recovery
The treatment for frozen shoulder aims to reduce pain and gradually regain mobility. The condition is often self-healing, but the right measures can speed up recovery and reduce discomfort during the process.
Physiotherapy: Individualized mobility exercises and stretching are central to gradually improving function.
Pain relief: Anti-inflammatory drugs or cortisone injections may be appropriate, especially in the painful phase.
Activity adjustment: It is important to keep the shoulder moving within the pain limit, but avoid overloading it.
In case of uncertain diagnosis or atypical symptoms, a MRI of the shoulder can be a valuable complement to confirm the diagnosis.
How can you test yourself if you have a frozen shoulder?
There are simple ways to get an idea of whether the symptoms are consistent with a frozen shoulder.
Test the mobility of the shoulder and shoulder:
A simple way to get an idea of whether you have a frozen shoulder is to compare the mobility between your shoulders in some basic movements.
1. Lift your arm straight up over your head - note if the movement stops earlier than on the other side or if pain occurs.
2. Rotate your arm outwards with your elbow next to your body - does the movement feel clearly limited or like a "mechanical stop" compared to the opposite side?
3. Try reaching behind your back, for example up towards the shoulder blade – is it difficult or impossible compared to the other shoulder?
With a frozen shoulder, it is common for several of these movements to be clearly limited, not only by pain but by actual stiffness in the joint.
Compare active and passive mobility:
If even passive mobility (when someone else moves your arm) is clearly limited, this strongly suggests frozen shoulder rather than an isolated muscle injury.
Typical pattern:
The combination of pain and pronounced stiffness in several directions of movement, especially outward rotation, is characteristic of frozen shoulder.
If you recognize these symptoms, it may be wise to seek medical evaluation to confirm the diagnosis and rule out other causes of shoulder discomfort.