What is spondylarthrosis?
Spondylarthrosis is a form of osteoarthritis that affects the small joints of the spine, called facet joints. The condition means that the cartilage in these joints gradually breaks down, leading to increased friction, inflammation and sometimes even bone spurs called osteophytes. It is a relatively common part of natural aging but can unfortunately cause problems in the form of both pain and stiffness.
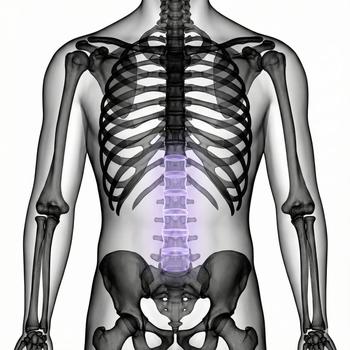
The facet joints are small joints that are located in pairs between the vertebrae along the entire spine. Together with the discs, they act as shock absorbers and control how the back can move, for example when bending, stretching and rotating. The joints also help to stabilize the spine and distribute the load between different structures.
When the facet joints are affected by osteoarthritis, mobility is reduced while the load on surrounding structures increases, which can give rise to pain, stiffness and in some cases even irritation of nearby nerve roots. This can lead to more widespread symptoms such as radiating pain, numbness or tingling depending on which structures are affected.
Spondylarthrosis most often occurs in the lower back (lumbar osteoarthritis) and the neck (cervical osteoarthritis), but can occur throughout the spine.
Why does spondylarthrosis occur?
The condition develops gradually when the cartilage in the facet joints breaks down. In cases where the cartilage thins or disappears completely, increased stress occurs on the joint surfaces, which can lead to pain and inflammation.
Contributing factors to spondylarthrosis include:
- Aging and natural wear and tear of the joints.
- Overuse or prolonged incorrect loading of the back.
- Previous injuries or disc changes.
- Impaired muscular stability.
- Excess weight, which increases the load on the spine.
Changes in the discs between the vertebrae can also contribute, as reduced disc height increases the load on the facet joints.
Symptoms of spondylarthrosis
Symptoms vary depending on where in the spine the changes are located and how pronounced they are. Spondylarthrosis can affect the entire spine but is most common in the lumbar and cervical spine. Many people have changes that are visible on X-rays or MRIs without having any obvious symptoms.
The pain is usually localized to the area where the changes are located:
- Lower back: Pain in the lower back, sometimes with stiffness and a feeling of fatigue in the back
- Thoracic back: More unusual, but can cause a dull pain between the shoulder blades
- Cervical back: Pain in the neck that can sometimes radiate to the shoulders or head
Common symptoms:
- Aching or local back or neck pain
- Stiffness, especially in the morning or after sitting still
- Pain that worsens with strain or bending backward
- Reduced mobility in the back
If bone spurs or swelling affect nerve roots, nerve-related symptoms may also occur. This can manifest as pain that radiates into the arms when the cervical spine is affected or into the legs when the lumbar spine is affected. Numbness or tingling is also common, and in some cases muscle weakness, depending on which nerve is affected.
How is the diagnosis made?
The diagnosis is based on a combination of symptoms, clinical examination and imaging. The doctor assesses the nature of the pain, mobility in the back and any neurological findings. An MRI scan is the most informative method when spondylarthrosis is suspected. MRI provides a detailed image of both soft tissues and bones and can show changes in the facet joints, discs, nerves and surrounding tissue.
Which part of the back is examined depends on where the symptoms are located. For lower back problems, MRI lumbar spine is often used, for pain between the shoulder blades, MRI thoracic spine may be appropriate, and for neck-related symptoms or radiation to the arms, MRI cervical spine is used.
MRI may be considered primarily when:
- Symptoms are long-lasting or severe.
- There is suspicion of nerve damage.
- Other causes of pain need to be ruled out.
X-rays can show skeletal changes such as reduced disc height and bone spurs, but provide less information about soft tissues. Computed tomography (CT) can be used in some cases to better visualize bone structures, but to avoid radiation, MRI is usually the first choice.
Treatment is carried out depending on symptoms and severity
The treatment of spondylarthrosis is adapted to the severity of symptoms and how much the condition affects everyday life. The goal is to reduce pain, improve function and prevent deterioration.
For mild symptoms, the following is often recommended:
- Physical activity and adapted training.
- Physical therapy to strengthen the muscles around the spine.
- Pain relief if necessary, such as paracetamol or NSAIDs.
In more severe cases, additional measures may be necessary:
- Specific rehabilitation and supervised exercise.
- Injections with local anesthetic and cortisone into the facet joints.
- Pain-modulating treatment.
In severe cases, where conservative treatment does not provide sufficient effect and where there is clear nerve damage, surgical treatment may be considered. This may, for example, involve relieving nerve structures or stabilizing parts of the spine.
Prognosis and course
Spondylarthrosis is a chronic condition that often develops slowly over time. Many people can live an active life with the right treatment and adaptation. Symptoms can vary in intensity and often occur in periods. With the right exercise and load adjustment, in many cases it is possible to significantly reduce the symptoms.
Living with spondylarthrosis
Living with spondylarthrosis often means finding a balance between activity and recovery. One of the most important factors in reducing the symptoms is to keep the back moving, as regular physical activity helps to maintain mobility, reduce stiffness and strengthen the structures that relieve the spine.
By avoiding prolonged sitting, strengthening the core muscles and adjusting the load in both work and everyday life, many people can experience a clear improvement in their symptoms. Ergonomics also plays an important role in reducing unnecessary strain on the back in daily life.
If the symptoms change, worsen or if neurological problems such as radiation, numbness or weakness occur, it is important to seek medical assessment for further investigation and treatment.