What is a rotator cuff tear?
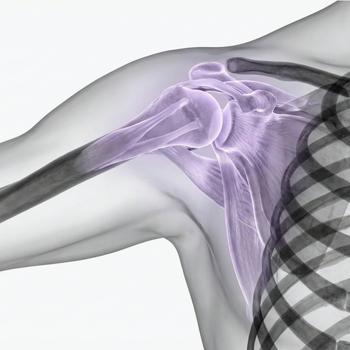
A rotator cuff tear is a partial or total tear of one or more of the tendons in the rotator cuff of the shoulder. The rotator cuff consists of four muscles (supraspinatus, infraspinatus, teres minor and subscapularis) whose tendons together stabilize the shoulder joint and enable controlled movements such as abduction, rotation and fine adjustment of the arm's position.
The shoulder joint (glenohumeral joint) has a unique anatomy with great mobility but limited bone stability. Stability is therefore largely dependent on soft tissues, especially the tendons of the rotator cuff. When a tendon tears, this finely tuned interaction is disrupted, leading to reduced force development, impaired joint function and often pain during load or movement.
What happens in the shoulder when a rotator cuff tear occurs?
A rotator cuff tear occurs when there is damage to the tendon attachment where the muscle normally attaches to the upper arm bone (humerus). This can happen suddenly, for example in a fall, or gradually through long-term overload and degenerative changes.
Tendon degeneration: With increasing age, the blood supply to the rotator cuff tendons, especially the supraspinatus tendon, decreases. This makes the tissue more vulnerable to micro-injuries that can develop into a larger tear over time.
Inflammation and pain: When the tendon is damaged, a local inflammatory reaction occurs. This leads to swelling and pain, especially during movement. The body tries to repair the damage, but the healing ability is often limited.
Altered biomechanics: When a tendon no longer functions optimally, the interaction between the muscles in the shoulder changes. This can lead to the upper arm bone sliding upwards, which causes impingement against the acromion and further pain.
Symptoms of a rotator cuff tear - how is the injury noticeable?
The symptoms of a rotator cuff tear can vary from discreet discomfort to pronounced functional impairment, depending on whether the injury occurred acutely or developed over time, and how extensive the tendon is affected. In many cases, the symptoms begin insidiously with increasing pain and weakness in the shoulder, while a larger rupture can cause a more sudden deterioration in both strength and mobility.
Pain in the shoulder: Often located on the outside of the shoulder and may radiate down the upper arm. The pain worsens when lifting the arm or putting weight on it.
Reduced strength: Especially when lifting above shoulder height or rotating the arm. In larger ruptures, it may be difficult to lift the arm at all.
Nighttime pain: Many people experience increased pain when lying on the affected side, which affects sleep.
Limited mobility: Stiffness and difficulty performing everyday activities such as getting dressed or reaching for shelves.
Causes of rotator cuff rupture
Rotator cuff ruptures most often occur through a combination of acute mechanical forces and long-term degenerative changes in the tendon tissue. The injury can therefore be divided into traumatic and degenerative causes, but in many cases these factors interact.
Trauma: Acute ruptures occur with sudden stress, for example when falling on an outstretched arm, jerking the arm or lifting a heavy object. This can lead to a direct rupture of a previously healthy or already weakened tendon.
Degenerative changes: The most common underlying cause is age-related degradation of the tendons. Reduced blood supply, especially to the supraspinatus tendon, leads to impaired healing and increased susceptibility to micro-injuries that can develop into a rupture over time.
Overload: Repeated movements above shoulder height, such as in certain professions (e.g. painters) or sports (e.g. tennis and throwing events), create chronic stress on the tendons and increase the risk of gradual degradation.
Subacromial impingement: Prolonged compression of the rotator cuff tendons between the humerus and acromion leads to mechanical irritation, inflammation and gradual weakening of the tendon structure, which can result in a rupture.
MRI or Ultrasound – how is a rotator cuff tear diagnosed?
The diagnosis of a rotator cuff tear is usually established using imaging diagnostics, where the choice of method is guided by both clinical suspicion and the information that needs to be obtained, but also from a financial perspective.
Ultrasound is usually used as an initial examination for shoulder complaints and provides the opportunity for a dynamic assessment where the tendons can be analyzed in real time during movement. This makes it possible to link findings to function and pain provocation in a clinically relevant way. The method is fast, accessible and cost-effective, and can identify both partial and total ruptures. At the same time, the examination is dependent on the experience of the examiner and can be more difficult to interpret in deeper structures or in patients with increased muscle mass.
MRI of the shoulder provides a more in-depth and complete mapping of the rotator cuff and is used when a more detailed assessment of the extent of the injury is needed, especially when larger ruptures are suspected or before treatment decisions. The method has a high level of detail and can clearly show the integrity of the tendon, the size of the rupture, any retraction and signs of muscle atrophy and fat deposition.
In addition to the tendons, MRI also enables a comprehensive assessment of the shoulder joint by visualizing other structures such as cartilage, bursae and joint capsule. This information is often crucial when planning treatment, not least before surgical procedures. The examination is also non-invasive, painless and is performed without the use of ionizing radiation.
What can you do yourself? Treatment and recovery
Treatment for rotator cuff tears is tailored to the extent of the injury, the severity of the symptoms and the individual's activity level. In many cases, treatment begins conservatively, with a focus on restoring function and reducing pain.
Physiotherapy: Individualized exercise is often the first-line treatment and aims to strengthen surrounding muscles, improve mobility and optimize the biomechanics of the shoulder.
Pain relief: Anti-inflammatory drugs can be used in the acute stage to reduce pain and inflammation.
Activity adjustment: Avoiding strenuous movements, especially repeated lifting above shoulder height, is important to reduce further irritation and enable healing.
Surgery: In the case of larger ruptures or persistent pronounced functional impairment, surgery may be considered after assessment by a specialist, especially if conservative treatment has not had sufficient effect.
In order to choose the right treatment strategy, a correct diagnosis is crucial. In the event of persistent pain or clear functional impairment, it may therefore be valuable to supplement with a MRI of the shoulder to obtain an accurate picture of the extent of the injury.
In many cases, a clinical assessment by, for example, a physiotherapist, naprapath or doctor can also be a first step in evaluating the symptoms and guiding further investigation.
In summary: Early investigation and individualized treatment are crucial for preserving the function of the shoulder and reducing the risk of long-term problems.