Quick version
A lumbar disc herniation is a common cause of sciatica and can lead to pain, numbness, and weakness in the leg. Most people, even those with large herniations, improve without surgery within 6–12 weeks.
MRI is central for confirming the diagnosis and showing how much a nerve is affected. Surgery is considered in cases of persistent severe pain, clear muscle weakness, or deterioration, and is required urgently if symptoms affect bladder or bowel function.
What is a large lumbar disc herniation?
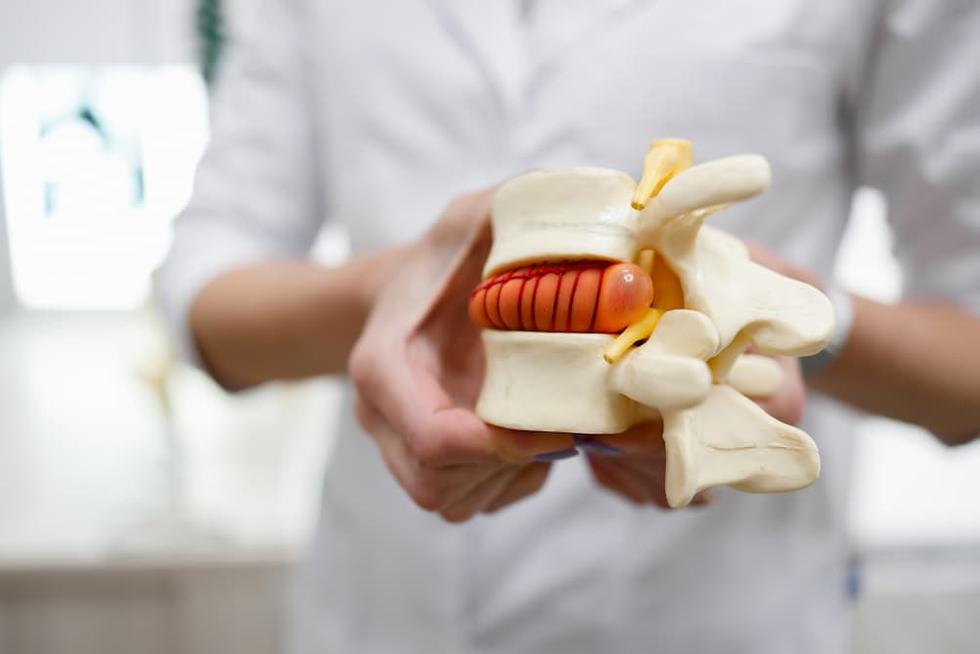
A herniated disc means that the soft core of an intervertebral disc is pushed out and affects a nerve in the spine. When this occurs in the lower back, it often leads to sciatica – a radiating pain from the back down into the leg. A large disc herniation means that a greater portion of the disc bulges out or has detached. However, it is not the size itself that determines how severe the symptoms are, but rather how much the nerve is affected.
What is the function of the discs?
The intervertebral discs act as shock absorbers between the vertebrae and allow the spine to be flexible. Over time, the discs become less elastic and more sensitive to strain, which increases the risk of cracks and herniation.
Common causes
Disc herniation often develops gradually as part of aging. A weakened disc may begin to bulge or rupture, sometimes in connection with strain such as heavy lifting or twisting movements. Lifestyle factors such as prolonged sitting and smoking can also affect disc health.
Symptoms of a large disc herniation
Symptoms vary depending on which nerve is affected, but leg pain is often more prominent than back pain. The pain typically radiates down the leg and may worsen with coughing, sneezing, or sitting. Numbness, tingling, and sometimes muscle weakness are also common, for example difficulty lifting the front of the foot.
In rare cases, nerves controlling the bladder and bowel are affected, which is a serious condition requiring urgent medical care.
How is a large disc herniation diagnosed?
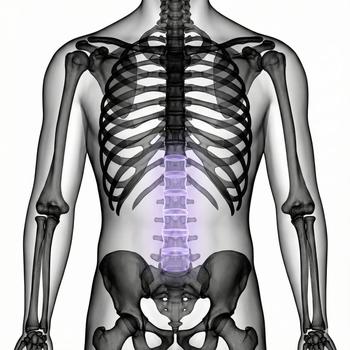
The diagnosis is initially based on your symptoms and a clinical examination where the doctor assesses strength, sensation, and reflexes. To confirm the diagnosis, a MRI (magnetic resonance imaging) of the lumbar spine is often performed, as it is the most reliable test when a disc herniation is suspected. MRI clearly shows the appearance of the disc and how the nerves are affected.
With the help of MRI, it is possible to:
- see exactly where the herniation is located
- assess its size
- determine if and how much a nerve root is compressed
- rule out other causes of the pain
MRI findings are always interpreted together with your symptoms. When imaging and symptoms align, the diagnosis becomes more certain and it is easier to determine the appropriate treatment.
MRI findings that may indicate the need for earlier treatment
Certain changes on MRI increase the likelihood that surgery may be needed sooner. This is especially true when a nerve is clearly compressed and this matches your symptoms. A sequestrated disc herniation, where a fragment of the disc has detached and lies freely, can cause more pronounced nerve involvement. Spinal canal narrowing can also worsen the symptoms.
When is non-surgical treatment sufficient?
Most disc herniations, even large ones, improve without surgery. The body can gradually break down the material pressing on the nerve, which reduces symptoms over time. Treatment focuses on relieving pain and keeping the body moving. This usually involves pain-relieving medications, adapted activity, and physiotherapy. Staying active, even at a low level, is important for recovery.
When should surgery be considered?
Surgery may be considered if leg pain is severe and persists despite treatment for approximately 6–12 weeks. This is especially relevant if the symptoms significantly limit daily life and if MRI shows clear nerve involvement. Progressive or persistent muscle weakness is also an important sign that surgery may be needed.
Emergency situations
Surgery is required urgently in cases of:
- bladder or bowel dysfunction
- numbness in the genital area
- rapidly worsening muscle weakness
Treatment and recovery
During surgery, the part of the disc that is pressing on the nerve is removed. Many people experience rapid relief of leg pain, but nerve recovery may take longer. After treatment, it is important to gradually return to activity and rebuild strength and mobility to reduce the risk of recurrence.