Quick version
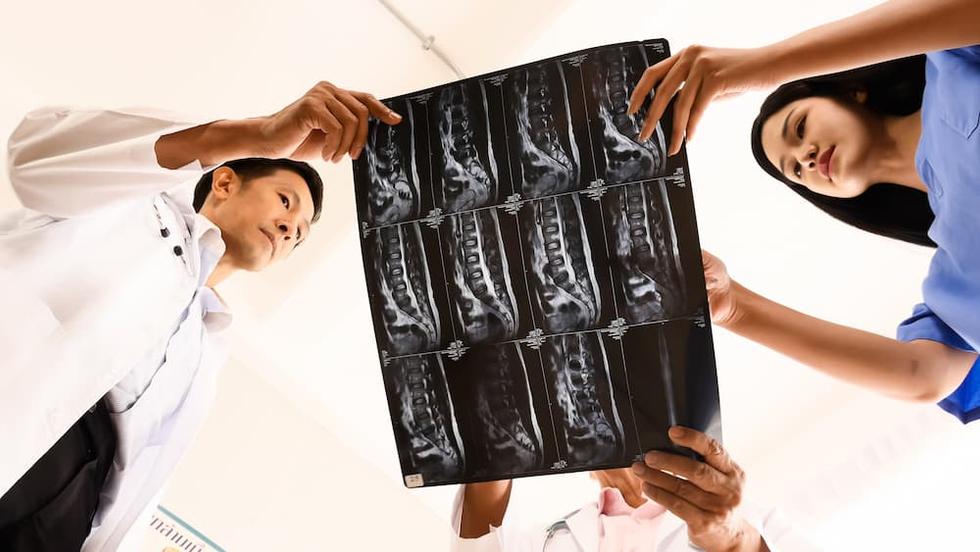
Degenerative changes in the spine are very common from middle age onward and are often seen even in people without pain. In most cases, they reflect the body’s natural aging process, where discs become drier, vertebrae change, and small bone spurs may form. The MRI findings themselves are therefore rarely dangerous. What matters is whether they correspond with your symptoms and what the clinical examination shows.
For mild or non-specific back pain, movement, exercise, and self-care are often sufficient. Only if the changes lead to clear nerve involvement—with radiating pain, numbness, weakness, or problems affecting bladder or bowel function—or if general symptoms such as fever and unexplained weight loss occur, is prompt medical evaluation and sometimes more extensive treatment necessary.
What do degenerative changes mean?
The word “degenerative” roughly means that something has changed or broken down over time. In the spine, it refers to wear-and-tear and age-related changes in the discs between the vertebrae, the vertebral endplates, and the small joints that stabilize the spine.
Disc degeneration means that the disc, which acts as a shock absorber between the vertebrae, gradually loses fluid and elasticity. It may become thinner and less flexible. Endplate changes describe alterations in the part of the vertebra closest to the disc. Osteophytes are small bone spurs that the body sometimes forms in response to strain and aging.
These types of changes increase with age and can be compared to wrinkles in the skin or gray hair—a sign that the body has been used, not necessarily that it is diseased.
Normal aging or something to worry about?
Many people over the age of 40–50 have degenerative changes on MRI without having any symptoms at all. Therefore, it can be misleading to assess the severity based solely on the imaging report. The changes become medically significant only when they cause symptoms, for example by pressing on a nerve or contributing to narrowing of the spinal canal. If the MRI findings correspond with your symptoms, they may be part of the explanation. If you have mild or non-specific back pain, however, the findings may be incidental—that is, visible on imaging but not causing problems.
What does this mean for your back pain?
Back pain is very common and is usually caused by several interacting factors. Muscles, joints, discs, posture, physical strain, stress, and sleep all affect how your back feels. Degenerative changes may sometimes contribute to stiffness and a dull ache, especially after prolonged sitting or standing. They may also be part of the explanation if you have long-standing symptoms.
If a nerve is affected, the pain may radiate into an arm or a leg and be combined with numbness or weakness. In such cases, it is not the “wear and tear” itself that is dangerous, but the pressure on the nerve that causes symptoms.
Common symptoms
Typical complaints associated with degenerative changes include a dull or aching pain in the lower back or neck and a feeling of stiffness, especially in the morning or after sitting still for a long time. Some people feel that their back is tired or unstable. If a nerve is involved, the pain may radiate down the leg or into the arm and may sometimes be accompanied by tingling, numbness, or reduced strength.
When should you seek medical care?
Most back problems are harmless and improve over time. However, you should seek medical care promptly if you experience sudden weakness in the legs or arms, difficulty controlling urination or bowel movements, numbness in the groin or around the anus, fever combined with back pain, or unexplained weight loss together with persistent pain. These symptoms may indicate a more serious condition that requires urgent evaluation.
If you have long-lasting pain that affects your work, sleep, or daily life, it is also wise to contact your primary care provider for an assessment.
Preventive measures
An active lifestyle is the best protection against long-term back problems. Regular exercise, strength training for the core and back muscles, reducing prolonged sitting, and maintaining good working posture are important factors. Quitting smoking is recommended, as smoking can negatively affect the discs’ nutrient supply and healing capacity.