Quick version
What Is Osteoarthritis?
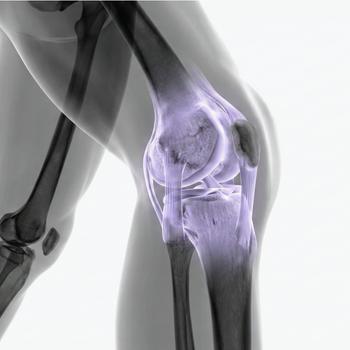
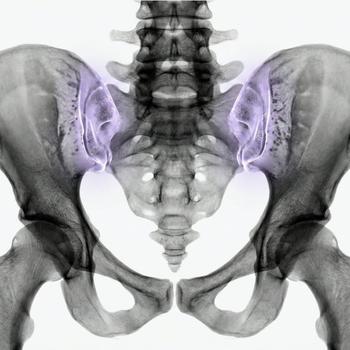
Osteoarthritis is a chronic joint disease that affects the cartilage in the joint. Cartilage is a smooth, shock-absorbing tissue that covers the ends of the bones and allows the joint to move smoothly. In osteoarthritis, the cartilage changes and the entire joint is gradually affected. This can lead to pain, stiffness, and sometimes swelling. Common symptoms include joint pain during weight-bearing activities, morning stiffness that eases after a while, and reduced mobility. Osteoarthritis most commonly affects the knees, hips, and hands. Many people searching for exercise for osteoarthritis have either been diagnosed or experience joint pain and suspect that it may be osteoarthritis.
Why Is Physical Activity for Osteoarthritis So Important?
It is common to worry that exercise will cause additional wear and tear on the joints. However, research shows that the right type of osteoarthritis exercise does not damage the cartilage. On the contrary, movement is essential for joint health. When you exercise, the muscles around the joint become stronger. This reduces the load on the joint itself. In knee osteoarthritis, strong thigh muscles can relieve stress on the knee joint. In hip osteoarthritis, strong gluteal muscles can improve stability and reduce pain. Movement also increases blood circulation and stimulates the joint cartilage. This can reduce the feeling of stiffness in the joints and help you move more naturally. In addition, exercise for osteoarthritis affects the body’s pain regulation system and may reduce low-grade inflammation in the joints.
What Type of Exercise Is Good for Osteoarthritis?
Effective exercise for osteoarthritis usually consists of a combination of strength training, cardiovascular training, and mobility exercises. The most important factor is that the training is regular and adapted. Strength training for osteoarthritis is particularly important. This may include simple exercises using body weight, resistance bands, or light weights. The goal is not to lift maximally heavy weights, but to gradually build strength and endurance in the muscles that support the joint. In knee osteoarthritis training, the focus is often on the thigh and hip muscles. In hip osteoarthritis training, the gluteal muscles and core stability are central.
Cardiovascular exercise is also an important part of physical activity for osteoarthritis. Low-intensity activities such as walking, cycling, or swimming are gentle on the joints while strengthening the heart and lungs. Walking with osteoarthritis can be adapted by choosing softer surfaces and a moderate pace. Cycling with osteoarthritis provides movement without heavy impact, and swimming with osteoarthritis reduces joint load thanks to the buoyancy of water.
Mobility exercises help reduce stiffness. These can be simple movements where the joint is taken through its natural range of motion without being pushed into pain. Balance training is particularly valuable for older adults, as it reduces the risk of falls and strengthens joint stability.
How Much Should You Exercise with Osteoarthritis?
General recommendations are at least 150 minutes of moderate physical activity per week, spread over several days. This could mean 30 minutes per day, five days a week. For people with osteoarthritis, it is wise to start gently and increase gradually. It is common to feel some soreness when beginning osteoarthritis exercise. A rule of thumb is that the pain should not be severe and should subside within 24 hours. If the pain increases significantly or persists for a long time, the load may need to be reduced. During rehabilitation for osteoarthritis, a physiotherapist can help develop an individualized exercise program. This can be especially valuable if you have pronounced knee osteoarthritis or hip osteoarthritis.
When Should You Seek Medical Care?
You should contact healthcare services if you have persistent joint pain that does not go away, if a joint suddenly becomes severely swollen and very painful, or if you experience redness and warmth in the joint. Such symptoms may indicate another type of joint inflammation or a different condition that requires assessment. Also seek care if symptoms worsen despite adapted exercise.
Examination and Diagnosis
The diagnosis of osteoarthritis is usually made through a clinical consultation and physical examination. The doctor or physiotherapist assesses mobility, pain, and function. X-rays are sometimes used to confirm joint changes, but symptoms are often more important than imaging findings.
Magnetic resonance imaging (MRI) can be valuable in certain situations. MRI provides a more detailed view of soft tissues, cartilage, menisci, ligaments, and bone marrow. The examination can detect early cartilage changes that are not visible on standard X-rays and can also show signs of inflammation or other joint injuries. MRI is particularly relevant if the symptoms are unclear, if the discomfort is disproportionately severe compared to X-ray findings, or if another injury besides osteoarthritis is suspected.
Treatment and Self-Care
Exercise for osteoarthritis is the foundation of treatment. In addition to physical activity, education about the condition, adjusting daily load, and, if necessary, pain-relieving medication may be appropriate. For people who are overweight, weight loss can reduce stress on the joints and relieve symptoms. It is important to view exercise as a long-term part of everyday life, not as a temporary effort. Regular physical activity for osteoarthritis provides the best results over time.
Prevention and Lifestyle
Although osteoarthritis cannot always be completely prevented, an active lifestyle can reduce the risk of severe symptoms. Keeping muscles strong, avoiding prolonged inactivity, and maintaining a healthy body weight reduce stress on the joints. Varying movement patterns and avoiding repetitive overuse are also important.
Related Conditions
Osteoarthritis can sometimes be confused with other joint diseases that cause joint inflammation, such as rheumatoid arthritis. The difference is that osteoarthritis is primarily a degenerative joint disease, while other conditions may be autoimmune and more systemic. When in doubt, medical evaluation is important.